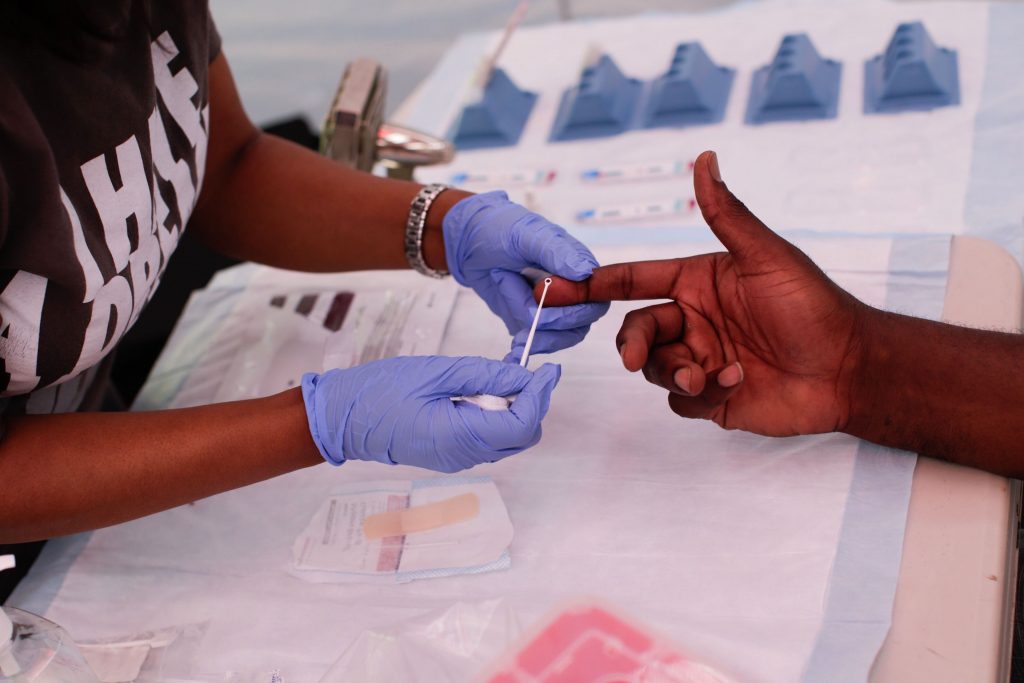
Critics Worry Government Surveillance of HIV May Hurt More Than It Helps
Robert Suttle has seen firsthand the legal risks of having HIV.
In 2008, Suttle said, a former partner accused him of not disclosing he was HIV-positive. He was charged under Louisiana law with “intentional exposure to AIDS virus.” Rather than fight the charge and risk a longer sentence, Suttle pleaded guilty, received a sentence of six months in state prison, and was required to register as a sex offender.
“You can be criminalized, certainly, for existing as a person living with HIV,” he said.
Suttle, who now lives in New York, said his experience has him worried about a new tool being promoted by federal officials to monitor the spread of HIV. With molecular surveillance, public health officials use routinely collected blood samples to identify how the virus is spreading among people.
Suttle said such data could be used in cases like his. “With this surveillance, you could be connected to many different people or considered to be the source that transmitted to all these other people,” he said.
Molecular surveillance is part of the Centers for Disease Control and Prevention’s HIV cluster detection and response program. It uses different kinds of surveillance data, including genetic changes in the virus, to identify networks of HIV transmission and tailor interventions to emerging outbreaks. HIV changes quickly, the CDC says, and finding similar viral strains in people can be a sign of rapid transmission.
Cluster detection and response is a pillar of the federal government’s 2019 plan to cut new HIV infections in the country 90% by 2030. Late last year, the Biden administration renewed its commitment to the program and then pumped an additional $115 million into the effort.
But molecular surveillance has met considerable opposition since it was rolled out nationally. Service providers, health equity advocates, and people living with HIV worry the risks of the approach outweigh the benefits, and their concerns have gotten louder as awareness of the tool grows. Some have called for the practice to stop until federal health officials address concerns about patient consent, data security, and the potential for HIV criminalization.
“This program — without having safeguards and guidances attached to it — has the real capacity to cause damage,” said Andrew Spieldenner, vice chair of the U.S. People Living With HIV Caucus, which has issued a formal call for the CDC to stop the practice.
One of the group’s main concerns involves consent. It says that many people living with HIV don’t know that genetic information about their strain of the virus could be used to link them to other people and that they would rather not have personal data used that way.
“The tension for me as a community member is neither the individual nor the community has consented,” said Alvan Quamina, executive director of NAESM, an Atlanta health nonprofit that focuses on serving Black gay men.
Viral genetic data has traditionally been used to test for resistance to HIV treatments, he said, and people don’t necessarily know about its use for surveillance. That has bred discomfort and fear about the program among service providers and people living with HIV, Quamina said. He added that those feelings can fuel stigmatization and keep people from seeking or keeping up with needed treatment.
“I think it absolutely can have a chilling effect on care engagement,” he said.
It’s a complication that comes as the effort to slow the spread of HIV has experienced substantial interruptions because of the covid-19 pandemic. In May, top CDC officials said the agency could fall short of its 2030 goal, in part because of a drop in HIV testing and because fewer people at risk of getting HIV are using preexposure prophylaxis, or PrEP, medication that reduces their chances of contracting the virus.
The CDC started requiring the state, territorial, and local health departments it funds to collect and submit HIV genetic sequences from people living with HIV in 2018, though some jurisdictions were already doing so.
The agency says jurisdictions must meet its standards for data security and shouldn’t use HIV genetic sequences to determine who may have infected whom or the direction of transmission between people.
But some advocates worry that the decentralized nature of the U.S. public health system — which puts the responsibility for running programs in the hands of local agencies — makes that data vulnerable to misuse.
In 2021, the CDC counted dozens of states with laws that criminalize HIV exposure. The agency called many of those statutes “outdated” and said they didn’t reflect the current scientific understanding of how the virus is transmitted.
Whether the surveillance strategy is more valuable than other, less invasive public health methods is unclear, said Catherine Hanssens, executive director and founder of the Center for HIV Law and Policy, which has raised concerns about possible criminalization and other risks associated with molecular surveillance. Hanssens cited alternatives such as campaigning for sexual health literacy and tracking new infections through patient interviews.
She questioned whether molecular surveillance is needed in areas where infections are high and public health officials know the groups most at risk. “Is the juice worth the squeeze?” she asked.
The CDC says molecular surveillance has helped detect about 300 HIV outbreaks across the country, most of which were previously unknown. But some state health officials — even those who see the value of the strategy — question whether it’s useful in every jurisdiction.
Dawn Fukuda, head of the office of HIV/AIDS at the Massachusetts Department of Public Health, said molecular surveillance helped her agency grasp the full scope of an HIV cluster among injection drug users in 2016. Having a more complete picture of the outbreak, Fukuda said, increased the urgency and scope of the state’s response.
Still, she acknowledged other states might not see the same benefits from molecular surveillance and might not have the money, workforce, or technology to fully implement the practice.
Samuel Burgess, the STD/HIV program director for the Louisiana Department of Health, said very few HIV clusters in his state have been detected using molecular surveillance, in part because the process of sequencing viral genetic data can take too long for the information to drive a quick reaction. Delays sometimes occur in HIV diagnosis and reporting, Burgess said, as well as in processing the data, sending it to the CDC for analysis, and waiting for the results.
In his state, Burgess said, public health officials already know who is most at risk of contracting HIV and the barriers they face in accessing care.
Dr. Alexa Oster, who leads the HIV cluster detection and response program at the CDC, has heard these concerns before. “We’re always happy to and interested in hearing the various perspectives about this work,” she said. “We feel that this type of dialogue and exchange can lead us towards a better place.”
Oster said local organizations and people involved in outbreaks have been more receptive to molecular surveillance than national HIV advocacy groups and highlighted a study that showed the strategy’s effectiveness in identifying clusters of rapid transmission.
Oster called molecular surveillance a “core public health function” and indicated the practice would not stop. But she said the CDC is open to considering how to allow local jurisdictions to tailor the program to their needs.
People with serious reservations about molecular surveillance think that engagement is crucial.
Tori Cooper directs community engagement for the Human Rights Campaign’s Transgender Justice Initiative and has spent years working with people living with HIV in Atlanta. She said some people concerned about the effort might be convinced of its benefits by focused and continued outreach.
“I believe that the onus now is on the CDC to do that, because there’s certain folk — there are a lot of folks — who are absolutely terrified,” she said.